Class 11 : Biology (In English) – Lesson 16: Excretory Products and Their Elimination
EXPLANATION & SUMMARY
🌱✨ Introduction
🧠 Excretion is the biological process of removing nitrogenous wastes and other harmful metabolic by-products from the body to maintain homeostasis.
🌿 All organisms produce metabolic wastes (like urea, CO₂, ammonia) during cellular respiration and other biochemical reactions.
⚙️ The excretory system collects, filters, and eliminates these wastes while maintaining water, ionic, and pH balance.
💡 Concept:
Excretion ≠ Egestion (which removes undigested food).
Excretion = removal of metabolic wastes produced inside cells.
💧 Excretory Products
During metabolism, organisms produce different wastes:
1️⃣ Ammonia (NH₃)
Highly toxic, requires large water for removal
Excreted by ammonotelic organisms (e.g., fishes, aquatic amphibians)
2️⃣ Urea
Less toxic, water-soluble
Excreted by ureotelic organisms (e.g., humans, mammals, amphibians)
3️⃣ Uric Acid
Least toxic, insoluble, excreted as paste
Seen in uricotelic organisms (birds, reptiles, insects)
🧬 Other wastes: CO₂, water, pigments, salts
💡 Concept: Type of nitrogenous waste depends on habitat and water availability.
🌾 Excretory Organs in Animals
Organism Excretory Structure
Amoeba Contractile vacuole
Platyhelminthes Flame cells
Earthworm Nephridia
Insects Malpighian tubules
Vertebrates Kidneys
🧠 In humans, kidneys are the main excretory organs.
🧍♂️ Human Excretory System
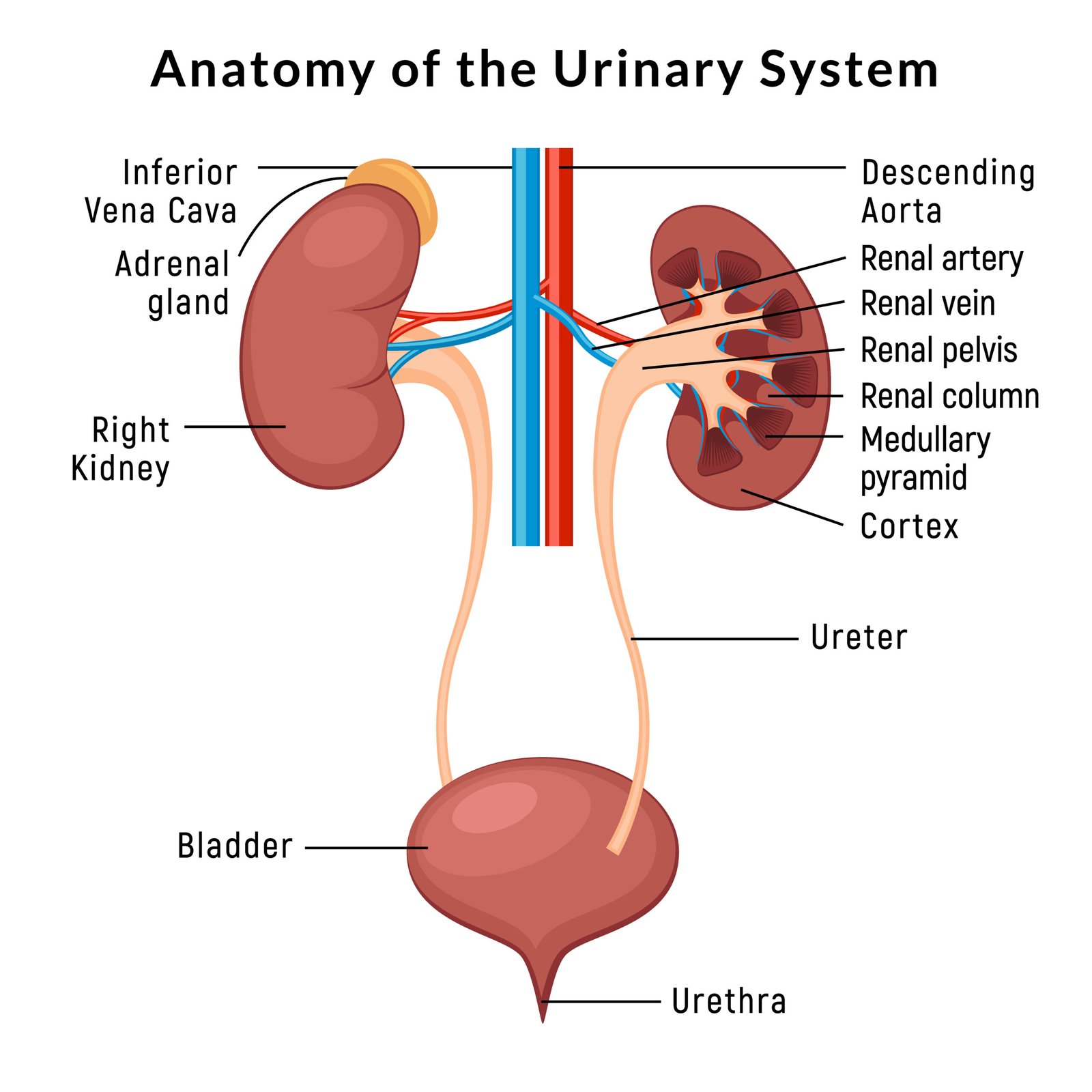
🩸 Composed of:
1️⃣ Kidneys (pair)
2️⃣ Ureters (pair)
3️⃣ Urinary bladder (storage)
4️⃣ Urethra (exit passage)
💡 Function: Filtration of blood, urine formation, and elimination.
🧬 Kidneys
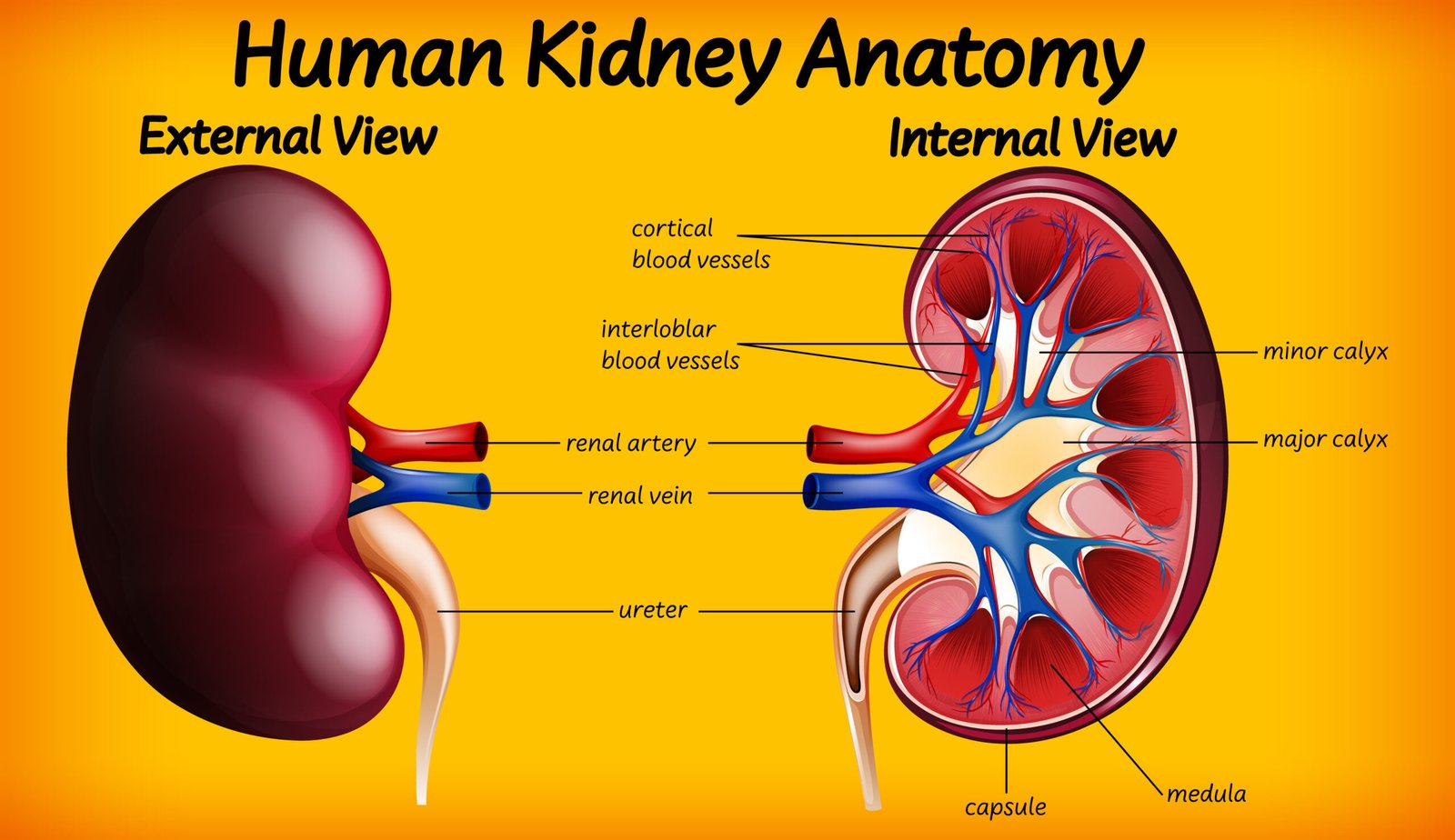
📘 Location: Retroperitoneal, one on each side of vertebral column
🫘 Shape: Bean-shaped
📏 Size: ~10–12 cm long
💧 Outer layer: Renal capsule
🧠 Internal structure:
Cortex (outer region)
Medulla (inner region) → contains pyramids
Pelvis → funnel-shaped cavity → continues as ureter
💡 Each kidney has ~1 million nephrons (structural and functional units).
🌿 Nephron
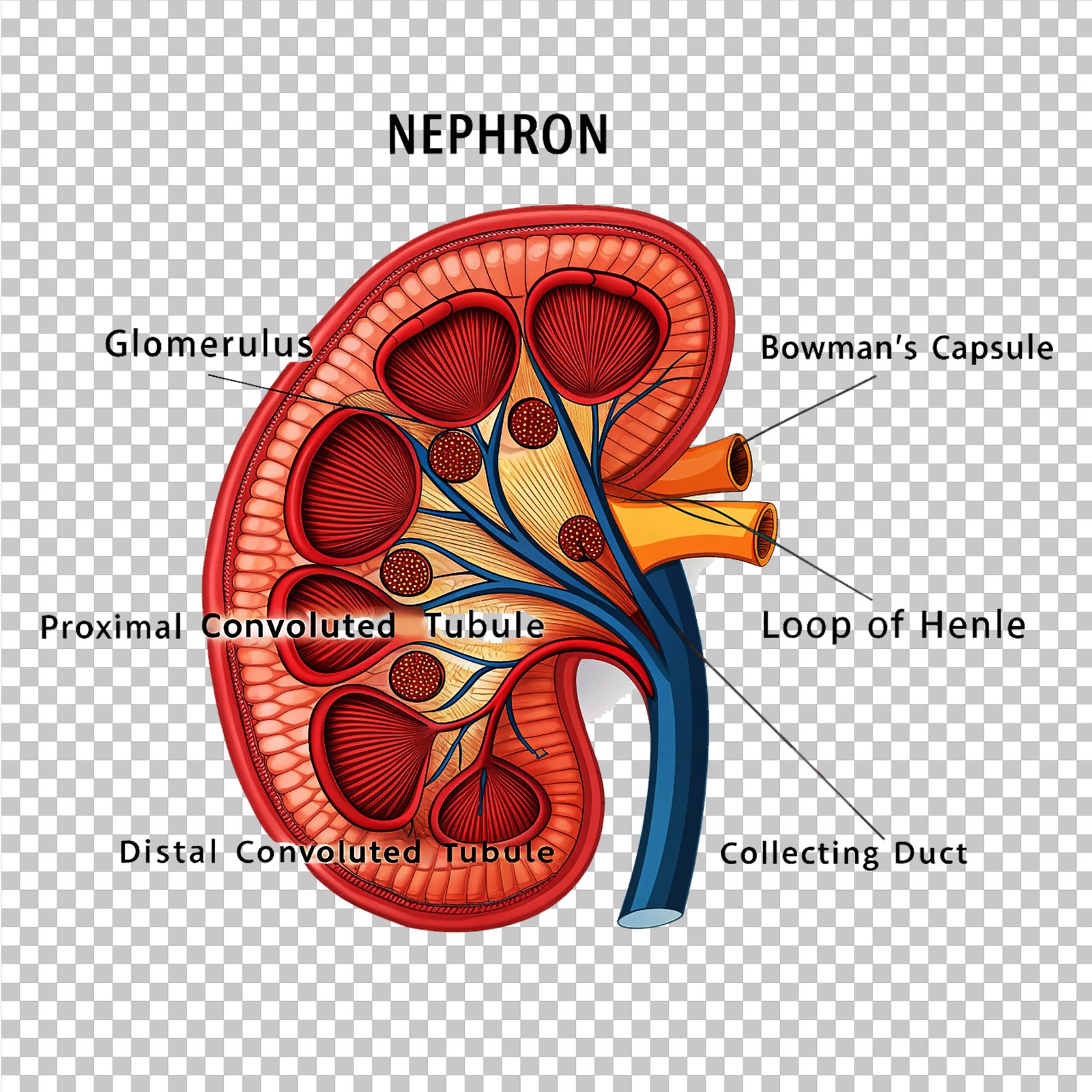
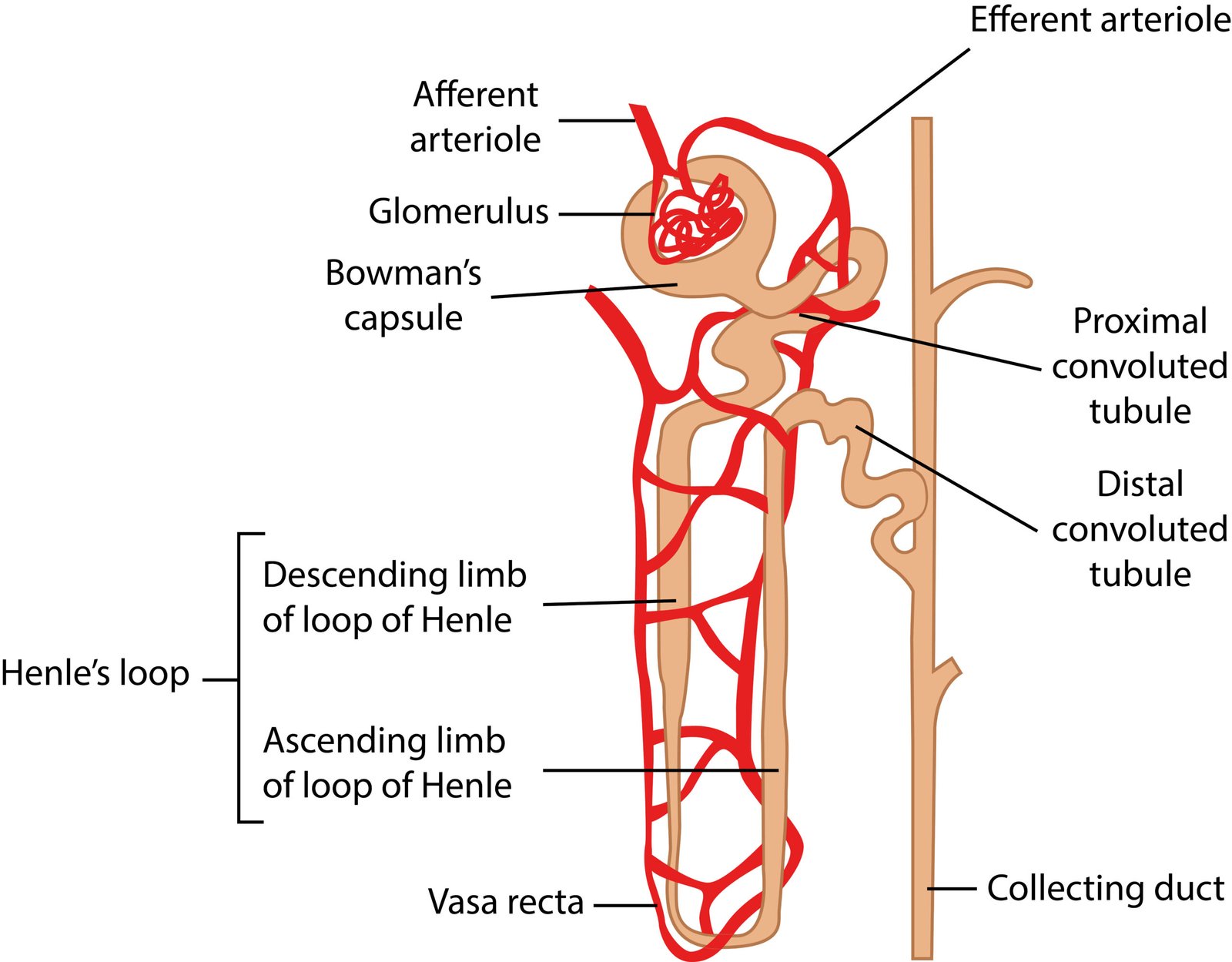
🧠 Parts:
1️⃣ Renal corpuscle → Bowman’s capsule + Glomerulus
2️⃣ Renal tubule → PCT, Loop of Henle, DCT
3️⃣ Collecting duct
💧 Glomerulus: tuft of capillaries from afferent arteriole
📘 Bowman’s capsule: cup-like structure enclosing glomerulus
💡 Function: Filtration, reabsorption, secretion → forms urine
⚙️ Steps of Urine Formation
1️⃣ Ultrafiltration
📍 In glomerulus
🧪 Blood pressure filters plasma → glomerular filtrate (water, salts, urea, glucose)
✏️ Note: Blood cells and proteins not filtered.
2️⃣ Selective Reabsorption
📍 In PCT, Loop of Henle, DCT
🌿 Useful substances (glucose, amino acids, ions) reabsorbed into blood
💧 ~99% filtrate reabsorbed
3️⃣ Tubular Secretion
📍 DCT and collecting duct
🧪 Additional wastes (K⁺, H⁺, NH₃) secreted into tubule
⚙️ Helps in acid-base balance
💡 Final product = urine
🌊 Mechanism Summary
Blood → Glomerulus → Filtration → Filtrate → Tubule → Reabsorption + Secretion → Urine → Pelvis → Ureter → Bladder → Urethra
🧪 Regulation of Kidney Function
🧠 1️⃣ Hormonal Control
💧 (a) Antidiuretic Hormone (ADH / Vasopressin)
Secreted by posterior pituitary
Increases water reabsorption in DCT & collecting duct
Low ADH → dilute urine (diuresis)
High ADH → concentrated urine
💡 Stimulus: Osmoreceptors detect ↑ blood osmolarity
⚡ (b) Aldosterone
Secreted by adrenal cortex
Promotes Na⁺ reabsorption, K⁺ secretion
Affects blood volume and pressure
🌾 (c) Atrial Natriuretic Factor (ANF)
Secreted by atria when BP ↑
Inhibits renin and aldosterone, promotes Na⁺ excretion
Lowers blood pressure
🧠 2️⃣ Neural Control
Hypothalamus regulates ADH secretion
Autonomic nervous system affects renal blood flow
🧪 Counter-Current Mechanism
🌀 Present in Loop of Henle and vasa recta
Maintains osmotic gradient in medulla
Enables concentration of urine
💧 Descending limb: permeable to water
💧 Ascending limb: impermeable to water, pumps ions
💡 Gradient helps in water conservation
💦 Composition of Urine
Water: ~95%
Urea: 2%
Ions: Na⁺, K⁺, Cl⁻
Creatinine, uric acid
📘 Normal urine volume: 1–1.5 L/day
📈 pH: ~6 (slightly acidic)
🚽 Micturition (Urination)
🧠 Process of urine expulsion from bladder
Controlled by nervous reflex
Stretch receptors in bladder → impulse to spinal cord → relaxation of sphincter
✏️ Note: Voluntary control develops in childhood.
🧠 Osmoregulation
⚙️ Maintenance of water and electrolyte balance
Kidneys regulate osmolarity via ADH, aldosterone
Dehydration → concentrated urine
Excess water → dilute urine
💡 Essential for homeostasis
⚠️ Disorders of Excretory System
1️⃣ Uremia: Accumulation of urea due to kidney failure
➡️ Treatment: Dialysis or transplant
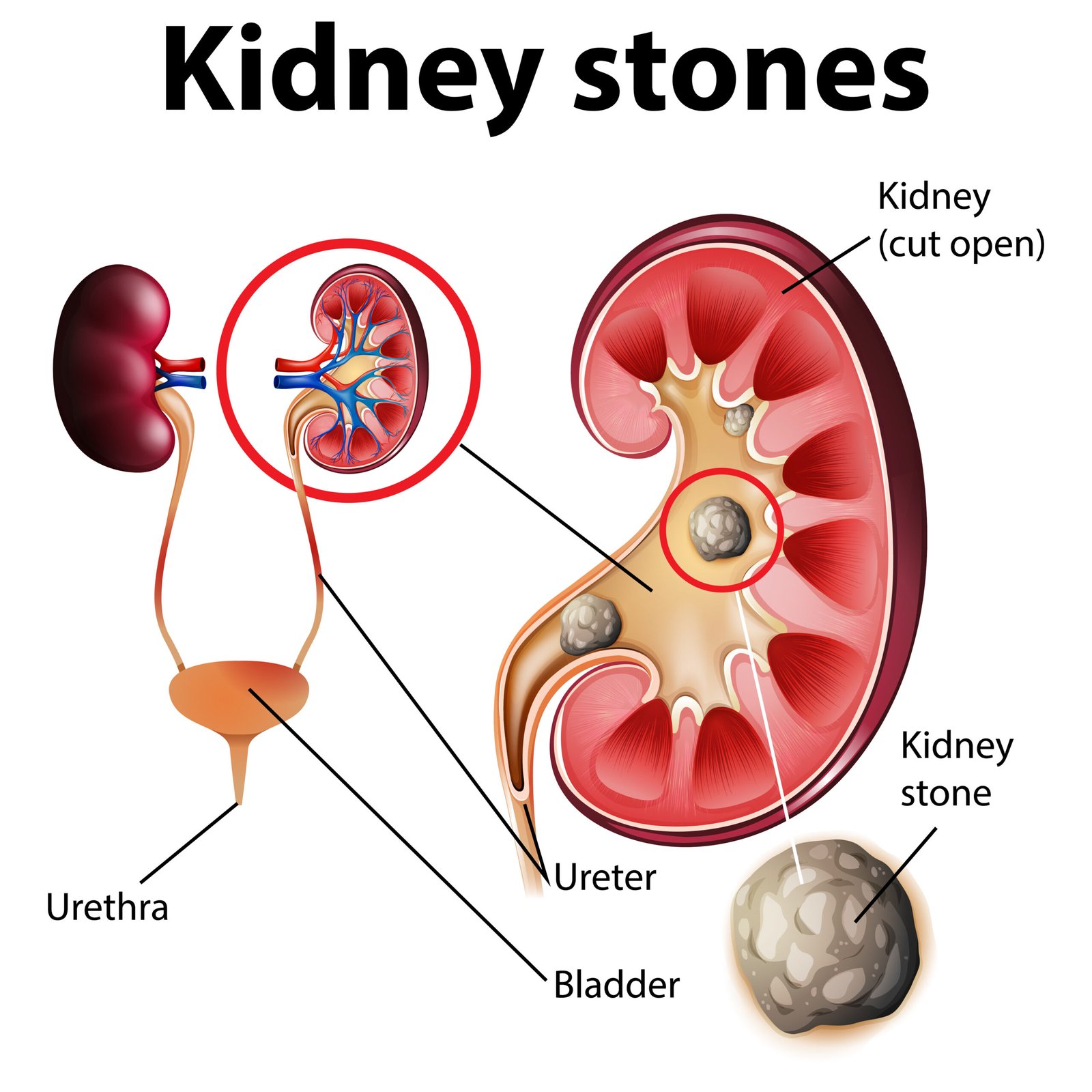
2️⃣ Renal Calculi: Kidney stones (Ca, uric acid)
➡️ Pain, obstruction
3️⃣ Glomerulonephritis: Inflammation of glomeruli
➡️ Reduced filtration
4️⃣ Diabetes insipidus: ADH deficiency → excess dilute urine
5️⃣ Oliguria/Anuria: Decreased/no urine output
💡 Prevention: Hydration, salt balance, regular check-ups.
⚙️ Artificial Kidney (Dialysis)
Used in renal failure:
Blood drawn → passed through dialyzer (semi-permeable membrane)
Waste diffuses out, clean blood returns
Temporary replacement for kidney function
🌍 Significance of Excretion
🧠 Removes toxic wastes
💧 Maintains fluid balance
⚡ Regulates pH and ions
🩸 Supports blood pressure stability
🌿 Ensures internal homeostasis
🌍 Why This Lesson Matters
💡 Explains how body maintains chemical balance
🧠 Foundation for renal physiology and medicine
⚙️ Basis of dialysis technology
🌍 Helps understand diseases like kidney failure, stones
📝 Quick Recap
🧬 Excretion = removal of metabolic wastes
💧 Products: ammonia, urea, uric acid
🩸 Humans: ureotelic → urea via kidneys
🫀 Organs: kidney, ureter, bladder, urethra
🧪 Steps: filtration → reabsorption → secretion
⚙️ Hormones: ADH, aldosterone, ANF
🌀 Counter-current aids concentration
💦 Urine: 95% water + urea + salts
⚠️ Disorders: uremia, stones, glomerulonephritis
🧠 Dialysis replaces kidney temporarily
📘 Summary
The excretory system in humans eliminates nitrogenous wastes, mainly urea, through the kidneys. Each kidney contains numerous nephrons that perform filtration, reabsorption, and secretion to form urine. Hormones like ADH and aldosterone regulate water and salt balance, maintaining homeostasis. The counter-current system in nephrons helps concentrate urine, conserving water. Disorders such as uremia and kidney stones disrupt function; dialysis aids in treatment. Excretion ensures the body remains chemically stable, supporting overall health and metabolism.
————————————————————————————————————————————————————————————————————————————
QUESTIONS FROM TEXTBOOK
🔵 Question 1. Explain the mechanism of urine formation.
🟢 Answer:
🧠 Urine formation occurs in nephrons through three main steps:
🌿 Glomerular Filtration
Takes place in Bowman’s capsule.
Blood is filtered under pressure → glomerular filtrate (water, glucose, salts, urea).
Called ultrafiltration.
🌸 Tubular Reabsorption
Selective reabsorption of useful substances (glucose, amino acids, Na⁺, water).
Occurs in PCT, loop of Henle, DCT.
Ensures conservation of essential materials.
💧 Tubular Secretion
Active secretion of H⁺, K⁺, NH₃ into filtrate.
Maintains acid-base balance.
✔️ Final urine = Filtrate – reabsorbed + secreted substances.
🔵 Question 2. What is meant by osmoregulation?
🟢 Answer:
🌿 Osmoregulation = maintenance of water and solute balance in body fluids.
💧 Kidneys adjust volume and composition of urine according to body needs.
💡 Hormones like ADH, aldosterone regulate water and salt reabsorption.
✔️ Ensures homeostasis of internal environment.
🔵 Question 3. Terrestrial animals are generally either ureotelic or uricotelic, not ammonotelic. Why?
🟢 Answer:
🧬 Ammonia is highly toxic and requires large amount of water for excretion.
➡️ Terrestrial animals cannot afford water loss.
🌿 Hence, they convert ammonia into urea (ureotelic) or uric acid (uricotelic), which are less toxic and require less water.
✔️ Adaptation for water conservation.
🔵 Question 4. What is the significance of juxtaglomerular apparatus (JGA) in kidney function?
🟢 Answer:
🧠 JGA is a special structure formed by DCT and afferent arteriole.
💡 Function:
Detects low blood pressure or sodium.
Secretes renin → activates RAAS pathway → produces angiotensin II.
➡️ Constricts blood vessels and releases aldosterone → increases Na⁺ and water reabsorption → raises blood pressure.
✔️ Maintains glomerular filtration rate (GFR) and blood pressure.
🔵 Question 5. Name the following:
🟢 Answer:
(a) 🌸 Excretory unit of kidney: Nephron
(b) 🌿 Protective covering of kidney: Renal capsule
(c) 💧 Capillary network inside Bowman’s capsule: Glomerulus
(d) 🧠 Part of nephron impermeable to water: Ascending limb of loop of Henle
🔵 Question 6. Fill in the blanks:
🟢 Answer:
(a) Bowman’s capsule + glomerulus = Malpighian body
(b) Reabsorption of glucose occurs in PCT
(c) ADH acts on collecting duct
(d) Counter-current mechanism is seen between loop of Henle and vasa recta
🔵 Question 7. What is the role of ADH in regulation of kidney function?
🟢 Answer:
💧 Antidiuretic hormone (ADH):
Secreted by posterior pituitary when osmolarity increases.
Increases water reabsorption from DCT and collecting ducts.
➡️ Produces concentrated urine.
✔️ In absence of ADH → dilute urine, dehydration.
🔵 Question 8. How does the kidney help in maintaining acid-base balance?
🟢 Answer:
⚖️ Kidneys regulate pH by:
Secreting H⁺ ions into filtrate.
Reabsorbing HCO₃⁻ into blood.
✔️ Maintains blood pH ≈ 7.4.
🔵 Question 9. Explain micturition and its regulation.
🟢 Answer:
🧠 Micturition: Process of urine release.
💡 Mechanism:
Urine collects in urinary bladder → wall stretches.
Stretch receptors send impulses to spinal cord.
Detrusor muscle contracts, sphincters relax → urine expelled.
✔️ Voluntary control develops with age.
🔵 Question 10. Mention any two excretory organs in human besides kidney.
🟢 Answer:
🌿 Lungs – eliminate CO₂ and water vapour.
🌸 Skin – excretes sweat (water, salts, urea).
⚗️ Liver – eliminates bile pigments (from haemoglobin breakdown).
🔵 Question 11. Differentiate between:
🟢 Answer:
Feature Cortical Nephrons Juxtamedullary Nephrons
Position Cortex Cortex-medulla boundary
Loop of Henle Short Long (extends deep)
Vasa recta Absent Present
Role Normal filtration Concentration of urine
🔵 Question 12. Explain counter-current mechanism in kidneys.
🟢 Answer:
💧 Loop of Henle and vasa recta form counter-current system:
Flow in opposite directions maintains osmotic gradient in medulla.
Enables water reabsorption → concentrated urine.
✔️ Driven by NaCl and urea transport.
🔵 Question 13. What is dialysis? When is it required?
🟢 Answer:
⚙️ Dialysis = artificial removal of wastes using dialyser.
➡️ Blood passed through semi-permeable membrane bathed in dialysing fluid.
➡️ Wastes diffuse out, useful solutes retained.
💡 Used in: Kidney failure or severe nephron damage.
————————————————————————————————————————————————————————————————————————————
OTHER IMPORTANT QUESTIONS FOR EXAMS
(CBSE MODEL QUESTIONS PAPER)
ESPECIALLY MADE FROM THIS LESSON ONLY
🔴 Question 1:
Which is the main nitrogenous waste in humans?
🔴1️⃣ Ammonia
🟢2️⃣ Urea
🟡3️⃣ Uric acid
🔵4️⃣ Creatinine
🟢 Answer: 2️⃣ Urea
🔴 Question 2:
Excretion is the process of —
🔴1️⃣ Removal of undigested food
🟢2️⃣ Removal of metabolic waste
🟡3️⃣ Removal of carbon dioxide only
🔵4️⃣ None of these
🟢 Answer: 2️⃣ Removal of metabolic waste
🔴 Question 3:
Functional unit of kidney is —
🔴1️⃣ Glomerulus
🟢2️⃣ Nephron
🟡3️⃣ Bowman’s capsule
🔵4️⃣ Collecting duct
🟢 Answer: 2️⃣ Nephron
🔴 Question 4:
The organ that forms urine in humans is —
🔴1️⃣ Liver
🟢2️⃣ Kidney
🟡3️⃣ Urinary bladder
🔵4️⃣ Ureter
🟢 Answer: 2️⃣ Kidney
🔴 Question 5:
Which part of nephron performs ultrafiltration?
🔴1️⃣ Loop of Henle
🟢2️⃣ Bowman’s capsule
🟡3️⃣ Collecting duct
🔵4️⃣ Distal tubule
🟢 Answer: 2️⃣ Bowman’s capsule
🔴 Question 6:
Which hormone regulates water reabsorption in kidney?
🔴1️⃣ Aldosterone
🟢2️⃣ ADH (Vasopressin)
🟡3️⃣ Insulin
🔵4️⃣ Cortisol
🟢 Answer: 2️⃣ ADH (Vasopressin)
🔴 Question 7:
What is the site of counter-current mechanism?
🔴1️⃣ Bowman’s capsule
🟢2️⃣ Loop of Henle and vasa recta
🟡3️⃣ Collecting duct
🔵4️⃣ Proximal tubule
🟢 Answer: 2️⃣ Loop of Henle and vasa recta
🔴 Question 8:
Which blood vessel brings blood to glomerulus?
🔴1️⃣ Efferent arteriole
🟢2️⃣ Afferent arteriole
🟡3️⃣ Renal vein
🔵4️⃣ Renal artery
🟢 Answer: 2️⃣ Afferent arteriole
🔴 Question 9:
Which of the following is not an excretory organ in humans?
🔴1️⃣ Kidney
🟢2️⃣ Lungs
🟡3️⃣ Skin
🔵4️⃣ Liver
🟢 Answer: 4️⃣ Liver
🔴 Question 10:
Which process helps maintain constant osmotic pressure in body?
🔴1️⃣ Ultrafiltration
🟢2️⃣ Osmoregulation
🟡3️⃣ Excretion
🔵4️⃣ Secretion
🟢 Answer: 2️⃣ Osmoregulation
🔴 Question 11:
Define excretion.
🟢 Answer:
The biological process of removing metabolic wastes (like urea, CO₂, salts) from the body is called excretion.
🔴 Question 12:
Name the main excretory organs in humans.
🟢 Answer:
1️⃣ Kidneys
2️⃣ Ureters
3️⃣ Urinary bladder
4️⃣ Urethra
🔴 Question 13:
Describe the main steps in urine formation.
🟢 Answer:
1️⃣ Ultrafiltration:
• In Bowman’s capsule; blood filtered under pressure.
• Forms glomerular filtrate (water, salts, urea, glucose).
2️⃣ Selective Reabsorption:
• In PCT, loop of Henle, DCT; essential substances (glucose, water, ions) reabsorbed.
3️⃣ Tubular Secretion:
• In DCT & collecting duct; H⁺, K⁺, NH₃ secreted into filtrate to maintain pH.
✅ Final product = urine, collected in renal pelvis.
🔴 Question 14:
Explain the structure of nephron.
🟢 Answer:
Parts:
1️⃣ Renal corpuscle: Bowman’s capsule + glomerulus.
2️⃣ Tubule:
– PCT: Reabsorption of nutrients.
– Loop of Henle: Counter-current mechanism.
– DCT: Selective secretion, ion balance.
– Collecting duct: Final concentration of urine.
💡 Nephron = structural & functional unit of kidney.
🔴 Question 15:
What is ultrafiltration? Where does it occur?
🟢 Answer:
Definition: Filtration of blood under pressure through glomerular capillaries into Bowman’s capsule.
Site: Renal corpuscle (Bowman’s capsule).
Cause: High glomerular blood pressure.
Result: Formation of glomerular filtrate (~180 L/day).
🔴 Question 16:
What is osmoregulation? Explain its role.
🟢 Answer:
Definition: Regulation of water and solute balance to maintain osmotic pressure.
Role:
1️⃣ Maintains fluid volume and ionic balance.
2️⃣ Controlled by hormones ADH and aldosterone.
3️⃣ Kidneys reabsorb or excrete water accordingly.
💡 Helps in homeostasis.
🔴 Question 17:
Explain the role of ADH in urine formation.
🟢 Answer:
ADH (Vasopressin): Secreted by posterior pituitary.
Functions:
1️⃣ Increases water reabsorption from DCT & collecting duct.
2️⃣ Reduces urine volume; makes it concentrated.
Deficiency: Causes Diabetes insipidus (excess dilute urine).
🔴 Question 18:
Describe the counter-current mechanism in kidneys.
🟢 Answer:
Structures involved: Loop of Henle & vasa recta.
Mechanism:
1️⃣ Descending limb: Permeable to water; water moves out.
2️⃣ Ascending limb: Impermeable to water; Na⁺/Cl⁻ actively transported out.
3️⃣ Vasa recta maintains osmotic gradient.
💡 Helps in forming hypertonic urine.
🔴 Question 19:
List the functions of kidney.
🟢 Answer:
1️⃣ Excretion: Removes metabolic wastes (urea).
2️⃣ Osmoregulation: Maintains water-salt balance.
3️⃣ Acid-base balance: Regulates pH by secreting H⁺/NH₃.
4️⃣ Hormonal function: Produces renin, erythropoietin.
5️⃣ Homeostasis: Maintains internal environment.
🔴 Question 20:
Explain the role of other organs in excretion.
🟢 Answer:
1️⃣ Lungs: Excrete CO₂ and water vapour.
2️⃣ Skin: Excretes sweat (water, salt, urea).
3️⃣ Liver: Excretes bile pigments, urea synthesis.
4️⃣ Large intestine: Expels salts and heavy metals.
💡 Assist kidneys in maintaining chemical balance.
🔴 Question 21:
What is micturition? Describe its control.
🟢 Answer:
Micturition: Process of urine expulsion from urinary bladder.
Steps:
1️⃣ Urine formed → stored in bladder.
2️⃣ Stretch receptors send signal to CNS.
3️⃣ Medulla coordinates contraction of bladder muscles, relaxation of sphincter.
💡 Involuntary in infants; voluntary in adults.
🔴 Question 22:
Differentiate between cortical and juxtamedullary nephrons.
🟢 Answer:
Feature Cortical Juxtamedullary
Location Cortex Near medulla
Loop of Henle Short Long
Vasa recta Absent/short Well-developed
Urine concentration Less High
💡 Juxtamedullary nephrons important for concentrated urine.
🔴 Question 23:
Describe the structure of the human kidney.
🟢 Answer:
Shape & Location: Bean-shaped, pair of organs located on either side of vertebral column.
Outer structure: Covered by fibrous capsule; has hilum for entry/exit of blood vessels and ureter.
Internal regions:
1️⃣ Cortex: Outer region with glomeruli.
2️⃣ Medulla: Inner region with renal pyramids.
3️⃣ Pelvis: Funnel-shaped cavity continuing as ureter.
Functional unit: Millions of nephrons perform filtration and urine formation.
💡 Function: Filtration of blood and maintenance of internal balance.
🔴 Question 24:
Explain the process of urine formation.
🟢 Answer:
1️⃣ Ultrafiltration:
• In glomerulus and Bowman’s capsule.
• Blood filtered under pressure → glomerular filtrate (~180 L/day).
2️⃣ Selective Reabsorption:
• In PCT, loop of Henle, DCT.
• Reabsorption of glucose, amino acids, water, Na⁺.
3️⃣ Tubular Secretion:
• H⁺, K⁺, NH₃ secreted into filtrate in DCT and collecting duct.
✅ Final urine: ~1.5 L/day, containing urea, salts, water.
🔴 Question 25:
Describe the role of nephron in excretion.
🟢 Answer:
Bowman’s capsule: Ultrafiltration.
PCT: Reabsorption of nutrients and water.
Loop of Henle: Maintains concentration gradient.
DCT: Ion exchange and pH regulation.
Collecting duct: Final adjustment of water, formation of urine.
💡 Together, nephrons maintain osmoregulation and homeostasis.
🔴 Question 26:
Explain the mechanism of osmoregulation in humans.
🟢 Answer:
Definition: Maintenance of water and solute balance.
Mechanism:
1️⃣ ADH release: From posterior pituitary when blood osmolarity ↑.
2️⃣ Increased water reabsorption from DCT and collecting duct.
3️⃣ Aldosterone: Reabsorbs Na⁺, excretes K⁺ → regulates salt balance.
4️⃣ Thirst mechanism: Stimulates water intake.
💡 Maintains constant blood osmotic pressure and volume.
🔴 Question 27:
Describe the hormonal control of kidney function.
🟢 Answer:
1️⃣ ADH (Vasopressin):
– Increases water reabsorption from DCT & collecting duct.
2️⃣ Aldosterone:
– From adrenal cortex; enhances Na⁺ reabsorption, K⁺ excretion.
3️⃣ ANF (Atrial Natriuretic Factor):
– From atria; inhibits renin & aldosterone, increases Na⁺ excretion.
4️⃣ Renin-Angiotensin system:
– Increases BP and promotes aldosterone release.
✅ These hormones coordinate kidney activity for homeostasis.
🔴 Question 28:
What is the role of liver, lungs, and skin in excretion?
🟢 Answer:
Liver:
– Converts ammonia → urea (urea cycle).
– Excretes bile pigments.
Lungs:
– Excrete CO₂ and water vapour.
Skin:
– Sweat glands remove water, salts, urea.
💡 These organs assist kidneys in maintaining chemical balance.
🔴 Question 29:
Describe the disorders related to excretory system.
🟢 Answer:
1️⃣ Uremia: High urea in blood due to kidney failure.
2️⃣ Renal calculi: Stone formation in kidneys.
3️⃣ Glomerulonephritis: Inflammation of glomeruli.
4️⃣ Diabetes insipidus: ADH deficiency; dilute urine.
💡 Severe uremia treated by dialysis or kidney transplant.
🔴 Question 30:
Explain the process of hemodialysis.
🟢 Answer:
Used in kidney failure to remove waste from blood.
Steps:
1️⃣ Patient’s blood passed through dialyzing unit.
2️⃣ Dialysis fluid: Contains same solute concentration as plasma except nitrogenous wastes.
3️⃣ Wastes (urea, uric acid) diffuse out; useful substances retained.
4️⃣ Clean blood returned to body.
💡 Temporary substitute for kidneys.
————————————————————————————————————————————————————————————————————————————
